Today’s Dietitian
Vol. 9 No. 9 P. 70
America. It’s the land of the free and the home of the super-sized soda, where the health of today’s children is at risk. The picture may be grim, but there’s hope for change through education and collaboration.
“During thousands of years marked by food scarcity, human beings developed efficient mechanisms to store energy as fat. Until recently, we rarely enjoyed the abundance of cheap food that we see today.”1
And enjoy we do. By some estimates, we experience an average of 5.6 eating episodes (ie, snacks and meals) per day.2 That could be translated to as many as 163,000 snacks and meals throughout our lifetime, totaling tons of food. Thus, dietary choices that we make can have a profound effect on overall health, especially for our children. Given the current trends, are we setting the stage for childhood obesity and poor oral health?
Influences on Early Eating Behaviors
Several factors influence what, when, and how often our children and adolescents eat. Today’s children glue themselves to the television more than ever before, according to recent research, and many children are watching between 21 and 28 hours of TV per week.3 This is more than twice what the American Academy of Pediatrics recommends.
Besides the obvious sedentary behavior, while watching television, children are receiving powerful advertising messages about foods. It comes as no surprise that advertisements aimed at youths are generally contrary to what is recommended for healthful eating.4 Adding to the concern is the fact that among some populations, roughly 38% of children aged 1 to 4 have televisions in their bedrooms.5 This encourages more TV viewing and less physical activity, while providing an even greater opportunity for advertising messages to influence preschoolers’ eating behaviors.
In addition to the influences of television, children are exposed to and often swayed by other children’s eating habits. They are exposed to snack machines and opportunities for frequent snacking, an abundance of convenience and fast foods, and super-sized servings. And, unfortunately, foods are frequently used as pacifiers that substitute for a lack of parental attention, time, or an understanding of the need for more nutritious foods.6 As a result, less nutritious foods are consumed more frequently.
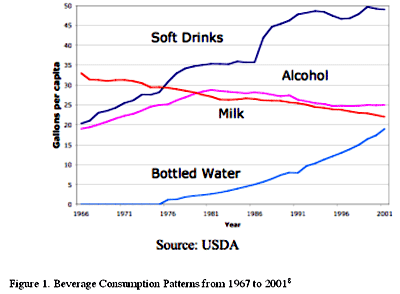
An example of children’s changing food habits can be seen in beverage consumption patterns (see Figure 1). Between 1970 and 2000, regular soda consumption climbed from 22 to 49 gallons per person per year. During that same period, milk intake dropped from 31 to 23 gallons per person per year. According to the U.S. Department of Agriculture’s (USDA) Continuing Survey of Food Intakes by Individuals (CSFII), 1994 to 1996, 20% of all children aged 1 to 2 consumed soft drinks.7 The USDA’s CSFII also shows that soda consumption exponentially increased through young adulthood (see Figure 1).8
Cause for Concern
Why should this be of worry? Because poor eating habits, including excess consumption of sweetened beverages, often lead to increased consumption of sugar and calories, which negatively affects the intake of various essential nutrients. Sweetened beverage intake is also associated with an increased risk of obesity and dental caries.9-11
Heavy soft drink consumption has been linked to low intake of magnesium, ascorbic acid, riboflavin, and vitamins A and D, as well as a high intake of calories, fat, and refined carbohydrates.7 Dietary surveys of teenagers found that in 1996, only one third of boys and girls consumed the number of servings of vegetables recommended by the USDA’s Food Guide Pyramid, less than 16% consumed adequate fruit servings, and 29% of boys and 11% of girls consumed the recommended servings of dairy foods.
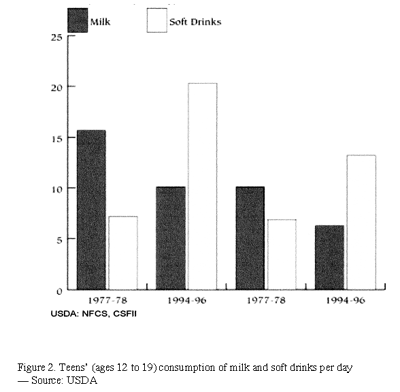
As shown in Figure 2, 30 years ago, teens drank twice as much milk as soft drinks. By 1996, those numbers reversed, such that young people drank twice as much soda as milk. There is no doubt that youths’ dietary inadequacies can increase risk factors for several diseases that manifest in adulthood (eg, osteoporosis).12
From Family-size to Super-size
A meta-analysis of research between 1966 and 2005 showed a positive correlation between a greater intake of sugar-sweetened beverages and weight gain in children and adults.9 In the 1950s, a family-size bottle of soda was 26 ounces. Today, a typical soft drink at fast-food restaurants is 12 to 42 ounces—for one person.
Of course, soda consumption is not the only calorie-dense item that has increased. McDonald’s shakes, Dunkin’ Donuts Coolattas, Starbucks’ Venti lattes, and even canned sweetened iced teas have become super-sized. And as portion sizes have grown, value marketing has skewed Americans’ thinking about appropriate portions. According to the American Institute for Cancer Research (AICR), value marketing appeals to the consumer’s desire for bargains by offering more (product) for less (money). The result: more calories attendant with less nutrient density.
Super-sized Consequences
What are some consequences of current eating habits for our nation’s youths? Between 1980 and 1994, the mean daily energy intake for children increased by approximately 100 to 300 kilocalories, while energy expenditure decreased (more television, computer usage, and video games and less physical activity), setting the stage for increased risk of obesity and associated diseases.
Based on the National Health and Nutrition Examination Survey (NHANES) II data of 1976 to 1980, only 5% of youths were classified as overweight. By the NHANES III survey, from 1988 to 1994, the number of overweight youths increased to 11%.13 More current estimates suggest that 25% of children in the United States are overweight and another 11% are obese.14 We know that overweight and obese children are at higher risk for cardiovascular disease, type 2 diabetes, asthma, gallbladder disease, and certain cancers.13,15-18
As children become more overweight, another health relationship has been observed: Increased obesity rates parallel increased caries rates.15,19,20 Clearly, a proper diet goes a long way toward reducing the risk for obesity and dental caries, particularly if we once again address types of foods consumed, frequency of exposure, and the amount of food eaten.21 More than 50 years ago, the classic Vipeholm study demonstrated what other, more current studies have supported: Carbohydrates, including sugars, have a role in caries formation; frequency of sugar consumption and duration of carbohydrate exposure also have a significant impact on dental health.22,23
Current health and nutrition behaviors among the nation’s youths seem to put them at risk for poor overall health. Childhood is the time for setting the stage for positive health outcomes.
Practical Solutions
What can be done? One answer lies in education, in raising the awareness of all those who influence children’s eating behaviors, including the family or main caregivers. It also includes all those who affect the health of children: parents, families, and caregivers; healthcare professionals; food industry and the media; educational authorities and schools; communities; and governmental agencies at all levels. Everyone must step up and set the stage for preventing childhood obesity and dental disease and promoting good overall health.
• Parents, Families, and Main Caregivers: It is important for all to understand how subtle messages impact what children learn. Nonverbal cues from primary caregivers, including what and how foods are purchased, prepared, served, and eaten, shape children’s habits.15 Research demonstrates that parents, families, and other main caregivers need to be more aware of their own eating behaviors and attitudes and the impact these may have on their children.24
Not surprising is that children’s preferences for high-fat, total fat, and sugar, as well as time spent in sedentary activities, have been positively associated with parental behaviors.25
Children who eat more family meals together generally eat more healthfully.26 A National Longitudinal Study of Adolescent Health concluded that parental presence at the evening meal is positively associated with adolescents’ higher consumption of fruits, vegetables, and dairy food.18 Nutrition and health professionals need to educate parents about the role of family mealtimes for healthy adolescent nutrition.
“Parents and caregivers of infants and children often receive little guidance about proper preventive dental and oral health care and dietary measures.”27 It is vital to teach all those involved in a child’s primary care about the value of good oral hygiene habits and dietary practices that “emphasize minimum exposure to retentive, fermentable carbohydrates, exposure to fluoridated water, and a varied, balanced diet that should continue throughout childhood.”27
Parents and caregivers also need guidance with children’s use of television, video games, and computers. The American Academy of Pediatrics recommends that parents set limits for their children, but families need to be educated more consistently about why and how this can be accomplished. It is not only that these inactivities encourage sedentary behavior but also that these media can and do deliver unhealthful messages.
In asking again what can be done, another equally important answer lies in collaboration, such as the following:
• Healthcare Professionals: Pediatric health professionals need to work with one another and parents to form a meaningful alliance resulting in the best possible healthcare for children.28 As an example of a simple way in which healthcare professionals can collaborate with families, body mass indexes should be routinely checked in children so that counseling and guidance can be provided to the families and/or caregivers.
Pediatricians, pediatric dentists, dietitians, and other healthcare advocates have a duty and an opportunity to be part of our children’s healthcare and prevention strategy team. Each brings a unique skill set to the equation and a chance to teach and learn from one another. Through collaboration, this strong alliance can help deliver a consistent message to parents and children: more nutrient-dense foods, less frequency of snacking, proper portion sizes, and adequate oral hygiene.
• Food Industry and the Media: The food industry could be a significant part of a collaborative effort to reduce childhood obesity, promote healthy eating, and prevent poor health outcomes. Think of how powerful their advertising efforts have been at influencing eating behaviors that we find today, and imagine how effective a change in their messaging could be.
Packaged foods and beverages could be more nutritious and nutrient dense; standard serving sizes could return to what they were before the 1980s; and packaging and advertising for the healthier dietary choices could entice the young consumer and replace what we find today with less-healthy packaged foods and beverages.
Restaurants, be they full-service or fast-food, could offer more realistic portion sizes and less super-sized meals; they could offer more nutritious choices and promote these in ways that would appeal to younger audiences. Nutritional information, while available today, could be made more accessible to parents and other caregivers.
Food labeling has been in existence since the early 1970s. From the beginning, the primary purpose of food labels was to be a teaching tool for the consumer. However, food labels need to be clearer and easier for the layperson to understand. Serving sizes of packaged foods also need to be more realistic.
The industry could collaborate with parents, families, schools, and healthcare providers by educating all of those involved with the health and well-being of our children.
• School Districts and Schools: School districts, as well as individual schools, have a unique opportunity to collaborate with families in delivering health-based messages. During the school year, the majority of a child’s day is spent in the classroom and elsewhere on campus. Thus, schools present an ideal venue for addressing a child’s health.29 Obviously, the concepts of health should be taught within the classroom, but the application of healthy lifestyles can be demonstrated in many ways: What foods and beverages are served to the students? What items are sold in the machines on campus? What physical activities are provided and promoted? A healthful school environment should be a top priority for the school districts and schools. Through collaborative efforts, the schools could work with families, healthcare workers, and communities to set the standards for good health.
An example of collaboration and education can be found within the California Dietetic Association (CDA). The CDA has formed a childhood obesity task force, partnering with the California School Boards Association. The task force is involved in monitoring and analyzing nutrition-related legislation, increasing overall participation in public policy making, and ensuring that children’s health issues remain a priority.
• Communities and State and Local Governments: Communities must rally together to keep children safe and provide opportunities for children to be involved and physically active. Are there places to safely walk, bike, run, or skate? Community coalitions could find creative ways to implement programs especially designed to promote healthy lifestyles and collaborate with state and local governments to garner their support.
• Federal Government: And finally, at the heart and soul of the charge is the federal government. Obesity prevention and the well-being of our youths must be a national public health priority. As an oversight body, the federal government can develop and promote high standards for health and fitness, enforce guidelines for issues such as advertising to children, be involved in funding prevention research, and convene national conferences aimed at collaborating with and educating those who affect the health of our children.
Summary
Certainly childhood obesity and poor oral health are complex in their etiologies. It therefore behooves us to take a multifaceted approach to finding successful solutions, all of which involve education and collaboration. Childhood must be the time for setting the stage to ensure that children develop healthy eating habits, appropriate levels of physical activity, and good oral hygiene habits that can last a lifetime.
— Terri Lisagor, EdD, MS, RD, is an assistant professor of nutrition and food science at California State University, Northridge, a registered dietitian in private practice, and a lecturer at the UCLA School of Dentistry.
References
1. Schlosser E. Fast Food Nation. New York: Houghton Mifflin Company; 2001.
2. Sepp H, Lennernas M, Abrahamsson L. Preschool children’s meal patterns analysed using the Food-Based Classification of Eating Episodes model. Scand J Food Nutr. 2006;50(3):131-138.
3. Davison KK, Marshall SJ, Birch LL. Cross-sectional and longitudinal associations between TV viewing and girls’ body mass index, overweight status, and percentage of body fat. J Pediatr. 2006;149(1):32-37.
4. Kotz K, Story M. Food advertisements during children’s Saturday morning television programming: Are they consistent with dietary recommendations? J Am Diet Assoc. 1994;94(11):1296-1300.
5. Dennison BA, Erb TA, Jenkins PL. Television viewing and television in bedroom associated with overweight risk among low-income preschool children. Pediatrics. 2002;109(6):1028-1035.
6. Lissau I, Sorensen TI. Parental neglect during childhood and increased risk of obesity in young adulthood. Lancet. 1994;343(8893):324-327.
7. Jacobson MF. “Liquid Candy — How Soft Drinks Are Harming Americans’ Health.” Center for Science in the Public Interest. 2005. Available here. Accessed October 17, 2003.
8. Diamond R, Moezzi M. “Changing Trends: A Brief History of the US Household Consumption of Energy, Water, Food, Beverages, and Tobacco.” Lawrence Berkeley National Laboratory. 2003. Available here.
9. Malik VS, Schulze MB, Hu FB. Intake of sugar-sweetened beverages and weight gain: a systematic review. Am J Clin Nutr. 2006;84(2):274-288.
10. Drewnowski A, Bellisle F. Liquid calories, sugar, and body weight. Am J Clin Nutr. 2007;85(3):651-661.
11. Ismail AI, Burt BA, Eklund SA. The cariogenicity of soft drinks in the United States. J Am Dent Assoc. 1984;109(2):241-245.
12. Gerrior S, Putnam J, Bente L. “Milk and Milk Products: Their Importance in the American Diet.” FoodReview: The Diet Quality Balancing Act. 1998. Available here.
13. Lytle LA. Nutritional issues for adolescents. J Am Diet Assoc. 2002;102(3):S8-S12.
14. Dehghan M, Akhtar-Danesh N, Merchant AT. Childhood obesity, prevalence and prevention. Nutr J. 2005;4:24.
15. Karp WB. Childhood and adolescent obesity: a national epidemic. J Calif Dent Assoc. 1998;26(10):771-773.
16. Wardlaw GM. Contemporary Nutrition: Issues and Insights. Boston: McGraw-Hill; 2003.
17. U.S. Health and Human Services. “Healthy People 2010: Understanding and Improving Health — Overweight and Obesity.” Available here.
18. Videon TM, Manning CK. Influences on adolescent eating patterns: The importance of family meals. J Adolesc Health. 2003;32(5):365-373.
19. Willershausen B, Haas G, Krummenauer F, et al. Relationship between high weight and caries frequency in German elementary school children. Eur J Med Res. 2004;9(8):400-404.
20. Al-Ansari JM, Al-Jairan LY, Gillespie GM. Dietary habits of the primary to secondary school population and implications for oral health. J Allied Health. 2006;35(2):75-80.
21. Ludwig DS, Peterson KE, Gortmaker SL. Relation between consumption of sugar-sweetened drinks and childhood obesity: A prospective, observational analysis. Lancet. 2001;357(9255):505-508.
22. Krasse B. The Vipeholm Dental Caries Study: Recollections and reflections 50 years later. J Dent Res. 2001;80(9):1785-1788.
23. Wan L, Lisagor T. “Dental perspectives: Rethinking Tricks and Treats.” California Pediatrician. 1993:48-49.
24. Hood MY, Moore LL, Sundarajan-Ramamurti A, et al. Parental eating attitudes and the development of obesity in children. The Framingham Children’s Study. Int J Obes. 2000;24(10):1319-1325.
25. Vauthier JM, Lluch A, Lecomte E, et al. Family resemblance in energy and macronutrient intakes: The Stanislas Family Study. Int J Epidemiol. 1996;25(5):1030-1037.
26. Gable S, Chang Y, Krull JL. Television watching and frequency of family meals are predictive of overweight onset and persistence in a national sample of school-aged children. J Am Diet Assoc. 2007;107(1):53-61.
27. Fitzsimons D, Dwyer JT, Palmer C, et al. Nutrition and oral health guidelines for pregnant women, infants, and children. J Am Diet Assoc. 1998;98(2):182-186,189s.
28. Nowak A. Oral health supervision during well-baby visits. In: Miller K (ed). Current Practices in Infant Feeding. Fremont, Mich.: Gerber Products Company, WIC Programs and Medical Services;1995:56-62.
29. Koplan J, Liverman C, Kraak V. Preventing childhood obesity: Health in the balance: Executive summary. J Am Diet Assoc. 2005;105(1):131-138.


