November 2015 Issue
November 2015 Issue
CPE Monthly: Probiotics May Prevent and Treat Clostridium difficile
By Mary Rodavich, MS, RD, LDN
Today's Dietitian
Vol. 17 No. 11 P. 46
Suggested CDR Learning Codes: 3100, 4040, 5220, 5270
Suggested CDR Performance Indicators: 8.1.2, 8.1.5, 8.3.6, 10.4.4
CPE Level 2
Take this course and earn 2 CEUs on our Continuing Education Learning Library
The prescription and administration of antibiotics, while beneficial in the treatment of many conditions, also can induce several adverse side effects. Antibiotics destroy bacteria in the gut, which may lead to abdominal discomfort and diarrhea. A common type of infection associated with antibiotic use is Clostridium difficile (C diff). It's a type of bacteria that attacks the lining of the intestines, resulting in symptoms ranging from mild to life threatening.
The number of C diff infections has been on the rise over the past decade, and deaths related to C diff increased by nearly 400% between the years 2000 and 2007. According to the Centers for Disease Control and Prevention, C diff infections are linked to 14,000 deaths in the United States every year.1 This dramatic rise may be related to poor infection control in health care settings, the increased use of antimicrobials and antibiotics, and the virulent ability of C diff spores to survive on environmental surfaces for many months.2 Economically, with the number of hospital stays from C diff infections tripling in the past decade, C diff costs Americans at least $1 billion in extra health care expenses every year.1
Nutrition professionals can play a major role in the prevention and treatment of C diff. Dietitians also can provide interventions to improve the nutritional status of C diff patients, who are twice as likely as others to have a diagnosis of malnutrition.3 One type of nutrition intervention is the dietary consumption of probiotics, which may aid in the recolonization of "good" bacteria in the gut.
This continuing education course reviews the evidence regarding probiotic consumption through diet and drugs in the prevention and treatment of C diff in the adult population.
What is C Diff?
Antibiotics are used to treat bacterial infections by killing or inhibiting the growth of microorganisms. While beneficial in the treatment of many conditions, antibiotic use also may produce several undesirable side effects. One of the most common is antibiotic-associated diarrhea, which occurs in 5% to 39% of patients, depending on the population and type of antibiotic. Diarrhea is characterized as frequent, loose, liquid stools (typically exceeding 300 mL) followed by the excessive loss of fluid and electrolytes, particularly sodium and potassium.4 Antibiotics may cause diarrhea by reducing the ability of colonic bacteria to convert osmotically active molecules (carbohydrates and amino acids) into gases and short-chain fatty acids (SCFAs). SCFAs help to facilitate the absorption of electrolytes and water from the colon. When there's a reduction in SCFAs, osmotically active molecules accumulate, leading to reduced absorption of electrolytes and water, resulting in diarrhea and fluid loss.5
C diff accounts for 20% to 30% of cases of antibiotic-associated diarrhea.2 One of the major risk factors for contracting C diff is long-term antibiotic use, which may kill the beneficial bacteria that are necessary to prevent the overgrowth of C diff. The risk of C diffincreases eight- to tenfold during the first month after antibiotic administration and threefold for the next two months after antibiotic administration.6 C diff is a spore-forming, anaerobic gram-positive bacteria that produces two pathogenic toxins: toxin A and toxin B. These toxins bind to the epithelial cells of the colon and catalyze the glucosylation of cytoplasmic proteins, which leads to an inflammatory response and eventual cell death.7
Once individuals contract C diff, they may spreadthe bacteria through contact with another person and via the fecal-oral route from a contaminated surface.6 Those most at risk of contracting the disease are older adults who have taken antibiotics and received medical care.1 Older adults are at a greater risk of C diff for several reasons, including age-related effects on the defense system (decreased gastric acidity and diminished antibody response to C diff toxins), the presence of underlying comorbidities, frequent use of antibiotics, repeated or prolonged hospitalizations (due to a more contaminated environment), and the use of acid suppressant medications, which increase the spores' ability to survive in the gastrointestinal [GI] tract. Many older adults with C diff are discharged from a hospital to a long term care facility. Environmental factors in these long term care facilities, which may further enable the spread of C diff, include shared rooms and restrooms, limited ability to isolate infected residents, and antimicrobial use. (C diff spores are resistant to alcohol, and antimicrobials may suppress normal bowel flora).7 Hospitals and long term care facilities can prevent the spread of the infection by isolating affected patients in single rooms (or a cohort of rooms), initiating contact precautions (visitors and clinicians must wear gloves and gowns upon entry into the room), and by practicing proper hand hygiene.2
About 20% of C diff culture-positive patients are asymptomatic. However, among the many common symptoms are abdominal discomfort, anorexia, nausea, colitis, fever, diarrhea, leukocytosis (elevated white blood cell count), hypoalbuminemia, and elevated serum creatinine.2
A serum albumin level less than 2.5 g/dL is associated with a poor prognosis in patients with C diff.6 C diff diarrhea may be resolved once the inciting antibiotic is discontinued; however, the wide range of symptoms may occur not only during the course of antibiotic use but also may present up to eight weeks after. Unfortunately, 15% to 35% of patients will experience a recurrence of symptoms within two months.2 Therefore, it's important for dietitians to aid in the prevention of a first occurrence of C diff as well as help to prevent recurrences.
Pharmacological treatment of C diff includes discontinuing the use of the inciting antibiotic as soon as medically able and avoiding the use of antiperistaltic agents, which may contribute to the retention of toxins in the intestines. Treatment also may include the intravenous or oral administration of the antibiotics vancomycin or metronidazole as well as the use of probiotics.2 In more rare but severe cases of C diff, surgical interventions, such as a partial or total colectomy, may be necessary.6
What Are Probiotics?
The term "probiotic" originates from the Greek language, in which the prefix "pro" means "in favor of," and the suffix "biotic" means "to pertain to life."8 While there's no standard definition of the term "probiotic," an expert panel at the Food and Agriculture Organization of the United Nations defined probiotics as "live microorganisms which when administered in adequate amounts confer a health benefit on the host."9
Health Benefits
There are many proposed health benefits of probiotics, including prevention of morbidity associated with necrotizing enterocolitis in preterm infants, regulation of intestinal transit and healthy gut function, regulation of the immune system, improvement in blood lipid composition, relief of irritable bowel syndrome symptoms, reduction of common upper respiratory tract infections, and prevention of antibiotic-associated diarrhea.10 The rationale for treating and preventing C diff with the consumption of probiotics is to restore the gut's microflora with "good" bacteria. The human intestine contains 100 trillion bacterial cells, comprising more than 400 different species of bacteria. Put into perspective, that's more than 10 times the number of cells composing the entire human body.11
Probiotics have a symbiotic relationship with the host's intestinal microbial ecosystem and stimulate both an immune and nonimmune response. While the exact mechanisms are still speculative and not fully understood, scientists believe probiotics may benefit the gut microbial environment by digesting food and competing for nutrients with pathogens, altering local pH to create an unfavorable environment for pathogens, scavenging superoxide radicals, stimulating epithelial mucin production, enhancing intestinal barrier functions, and competing for adhesion with pathogens.12
It's important to note that there are other types of beneficial microorganisms, known as prebiotics and synbiotics. Prebiotics are nondigestible food ingredients that stimulate the growth and/or activity of bacteria in the colon. Synbiotics are food or supplements that contain both probiotics and prebiotics, working synergistically to benefit the host.13 For the purpose of this article, the focus is solely on probiotics.
Dietary Sources
It's believed that humans began making fermented milk products as early as 7000 BC in an attempt to preserve milk; however, the first commercially produced yogurt, made by Danone in Madrid, Spain, didn't appear until 1922. During the fermentation of milk products, much of the lactose is converted to lactic acid. This process results in lower lactose levels, which is why many individuals with lactose malabsorption can tolerate these products better than they can tolerate milk. The protein in fermented milks also is better digested by the human gut due to the proteolytic effects of the starter bacteria, creating higher levels of peptides and amino acids.14
Dietary sources of probiotics include fermented milk products (such as yogurt, kefir, and buttermilk), fermented vegetables (such as kimchi and sauerkraut), and fermented soy products (such as miso and tempeh).5 There also are numerous types of probiotic products on the market, including food products, meal replacements, dietary supplements, neutraceuticals, over-the-counter drugs, and prescription drugs. Products in the form of a tablet, capsule, or sachet contain probiotic bacteria that have been freeze-dried.12 Consuming probiotics through food sources as opposed to supplements is recognized as a better choice due to the synergistic effect between probiotics and other nutrients found in food.11
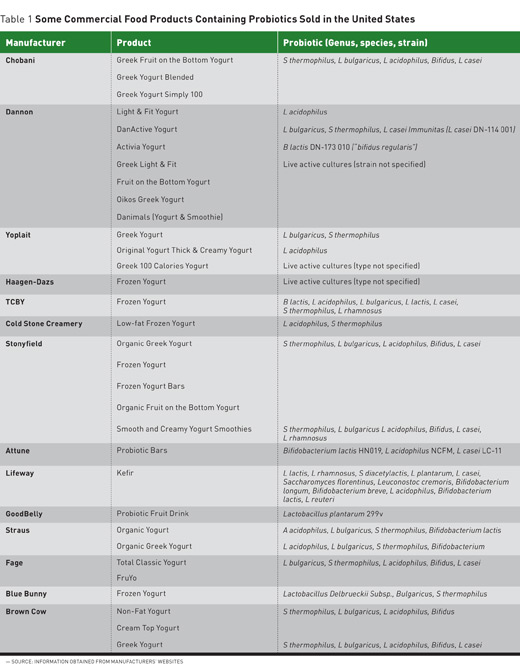
The most common probiotic species used in commercial products are Lactobacillus species, Bifidobacterium species, Streptococcusspecies, and yeasts (Saccharomyces boulardii).11 Table 1 lists some commercial food products containing probiotics that currently are sold in the United States.
Choosing a Probiotic Product
The specific dosage needed to produce noticeable health benefits varies greatly depending on the type of strain and the product. Many over-the-counter products provide 1 billion to 10 billion colony-forming units (CFU) per dose.12 The shelf life of probiotics is about three to six weeks for refrigerated products and about 12 months for dried supplements. Because probiotics are sensitive to environmental factors such as heat, moisture, oxygen, and acid, it's recommended to consume products as close to the manufacturing date as possible.13
Probiotics exert their effects as they metabolize while passing through the gut. Therefore, daily consumption is considered the best way to maintain their health benefits.11 Despite the fact that probiotics are destroyed by heat and acidity, they do have the ability to survive transit through the human GI tract. Some of the conditions that determine the extent of probiotic survival through the gut include the degree of stomach acidity, the length of exposure to acid, and the concentration and exposure to bile salts. Many probiotic strains survive the GI tract at a rate of 20% to 40% and can enter the colon in a viable state to beneficially affect its microecology.15
As the public learns more about the benefits of probiotics, global sales of probiotic products are projected to reach $42 billion in 2016.16 According to a large survey, public awareness that probiotics can be beneficial for maintaining a healthy digestive system increased from 58% to 72% from 2007 to 2011. In this survey, 38% of individuals already were consuming probiotics in yogurt or other products fortified with beneficial cultures, and 47% were likely or somewhat likely to consume these products.17 This indicates that the public is aware of the benefits of probiotics and is at least willing to try a probiotic-containing food. Americans are consuming less yogurt than individuals in many other countries. Yogurt consumption in Europe accounts for nearly 32% of total dairy intake compared with only 5% in the United States.13 Nutrition professionals can help educate clients and patients and encourage them to try probiotic-containing foods, especially yogurt, which is one of the most abundant dietary probiotic sources. Dietitians should encourage patients to choose probiotic products that are lower in fat (≤3 g of fat per serving) and contain little added sugar (≤10 g of sugar per serving).18
To help consumers recognize yogurt products with significant amounts of probiotics, the National Yogurt Association established a Live & Active Culture seal. It can be found on product packaging when the yogurt meets specific requirements. Refrigerated yogurt must contain 100 million viable lactic acid bacteria per gram at the time of manufacture, and frozen yogurts must contain 10 million viable lactic acid bacteria per gram at the time of manufacture.19 Many yogurts contain both starter cultures and additional beneficial, probiotic bacteria (such as Lactobacillus or Bifidobacteria). Therefore, the Live & Active Cultures seal is a good indicator of probiotics, but caution may be needed because it doesn't distinguish starter culture bacteria from probiotic bacteria.13
There are hundreds of commercial yogurt products from which consumers can choose, such as whole milk, low fat, nonfat, plain, flavored, inclusion of fruit, and the addition of artificial sweeteners. Another increasingly popular type of yogurt is Greek yogurt. It's made by straining the fermented milk after coagulation; this removes the liquid whey and some of the lactose, creating a richer consistency. Greek yogurt is lower in fat and higher in protein than regular yogurt. To be considered Greek-style, yogurt must contain at least 5.6% protein (% m/m), compared with 2.7% found in regular, strained yogurt.20
The FDA has declared many food sources of probiotics generally recognized as safe for the public.11 Dietitians can encourage high-risk clients and patients to include probiotic-rich foods in their diets by reinforcing the proposed health benefits. For consumers, probiotic foods are low in cost, easy to try, and exert very few adverse side effects. Some minor side effects that have been reported include thirst, constipation, bloating, flatulence, nausea, vomiting, abdominal pain, rash, and diarrhea.10 Individuals who are immunocompromised, recovering from surgery, or have compromised gut integrity are at a greater risk of infection and should consume probiotics only under medical supervision.13
Other Health Benefits of Fermented Milk Products
Recommending yogurt and fermented milk products can be a simple way for dietitians to promote probiotic intake. For consumers, these products are easily accessible, are high in nutrient density, provide high-quality protein, are easily digestible, and can be flavored based on personal preference. According to the USDA nutrient database, a typical 6-oz serving of plain, low-fat yogurt contains approximately 100 kcal, 9 g protein, and 3 g fat. It meets 40% of the dietary reference intake (DRI) for vitamin B12, 35% of the DRI for phosphorus, 30% of the DRI for calcium, 20% of the DRI for pantothenic acid, and 10% of the DRI for potassium (for adults).21 Yogurt is an easy medium in which clients can mix in other foods (such as granola, nuts, seeds, fruits, cold cereals, graham crackers, honey, cinnamon, jams, and peanut butter), which add texture and other beneficial vitamins and nutrients.
Another benefit of yogurt is that it has been shown to decrease the incidence of overweight and obesity. In one study, individuals who consumed seven or more servings of yogurt per week exhibited a significantly lower risk of becoming overweight or obese compared with those in the lowest category (two or less servings per week) (P≤0.001).22 Yogurt consumption is also associated with better diet quality. In a cross-sectional study, yogurt consumers had a better Dietary Guidelines Adherence Index score (a score of diet quality) compared with nonconsumers. Yogurt consumers also had greater potassium intakes and were less likely to have inadequate intakes of vitamin B2, vitamin B12, calcium, magnesium, and zinc (all P<0.001). In addition, yogurt consumption was associated with lower levels of triglycerides, glucose, systolic blood pressure, and insulin resistance (all P<0.05). Thus, the authors of this study concluded that yogurt can aid in improving overall diet quality, helping consumers achieve greater intake of many nutrients and maintain metabolic well-being.23 In another study, however, yogurt consumption did not significantly improve health-related quality of life scores, a global indicator of perceived health status.24
Antibiotic-Associated Diarrhea and Probiotics
Antibiotic-associated diarrhea is becoming an increasingly common complication of antibiotic use. There's evidence that probiotics can help in the prevention and treatment of generalized antibiotic-associated diarrheaas well as C diff, the most common type of antibiotic-associated diarrhea
In one study, elderly hospitalized patients receiving oral or intravenous antibiotics consumed two 8-oz containers per day of probiotic-containing yogurt or received no yogurt. After eight days of treatment, subjects who consumed yogurt reported significantly less frequent diarrhea (12% vs 24%) and significantly less total diarrhea days (23 vs 60 days) compared with those who received no yogurt. In those patients reporting diarrhea, the duration was 31% shorter among subjects receiving yogurt compared with control subjects (1.8 vs 2.6 days, respectively, P=0.08). In addition, subjects in the yogurt group didn't report any negative side effects from its consumption.25
In a randomized, double-blind study, healthy subjects receiving antibiotics consumed two 4-oz containers per day of yogurt that contained Lactobacillus acidophilus LA-5, Bifidobacterium lactis BB-12, and Streptococcus thermophilus (>106 CFU/g each). After five weeks of treatment, subjects who consumed yogurt had significantly reduced duration of watery stools due to antibiotics compared with control subjects (four vs 10 days, P<0.05).26
In another study, patients who were receiving antibiotic treatment were randomized into one of three intervention groups: those consuming 5 oz of bio yogurt (S thermophilus, L acidophilus, B anamalis subsp. lactis), 5 oz of commercial yogurt (S thermophilus, L delbrueckiisubsp. bulgaris), or no yogurt. After 12 days, the rates of diarrhea were not statistically significant between the three groups. However, in patients who previously had an episode of antibiotic-associated diarrhea in the past, the rate of diarrhea was 20% for the bio yogurt group, 4% for the commercial yogurt group, and 38% for those who had no yogurt (p=0.03). These results indicate that yogurt consumption may prevent the recurrence of antibiotic-associated diarrheain individuals who have a previous history of the condition. Results also may have been affected by this study's use of a relatively small dose of 5 oz of yogurt daily.27
C diff and Probiotics
As discussed, the most common type of antibiotic-associated diarrhea is C diff. In a scientific survey, 98% of gastroenterologists believe that probiotics have a role in the treatment of GI illness, and 60% believe the literature supports probiotic use for the treatment of C diff.28
When a patient with or at high risk of developing C diff is ordered an antibiotic regimen, probiotic drugs and supplements often are prescribed for one to three weeks longer than the duration of antibiotic treatment. It's also recommended that these products be consumed with food because decreased stomach acidity provides a more favorable environment to allow probiotics to reach the intestines.29
In a large meta-analysis of 20 randomized trials, adults who received probiotics had a 78% lower incidence of C diff-associated diarrhea (CDAD) compared with control groups (relative risk=0.22). Adverse effects, such as abdominal cramping, nausea, fever, flatulence, and taste disturbances, were found in 9.3% of the probiotic groups vs 12.6% of the control groups.30 Another meta-analysis of 16 randomized controlled trials found a 63% decreased risk of CDAD in hospitalized patients receiving probiotics compared with control groups (relative risk=0.37). Most of the probiotic formulations used contained Lactobacillus and S boulardii species, and a typical follow-up period for patients was less than four weeks.31
In a dose-response study, inpatient subjects receiving antibiotic treatment were randomized into one of three treatment groups: those receiving high-dose probiotics (1.70 X 10 billion CFU), low-dose probiotics (4.17 X 1 billion CFU), or placebo. The probiotic capsule contained four strains: L acidophilus NCFM, L paracasei Lpc-37, B lactis Bi-07, and B lactis Bl-04. The incidence of CDAD was the same, 1.8%, in both the low-dose and high-dose probiotic groups, and 4.8% in the placebo group. Even though the incidence was the same in both probiotic groups, statistical significance was found only in the high-dose probiotic group compared with placebo.32
In a similar dose-response study, older adults on antibiotic therapy were randomized into one of three groups: those receiving two probiotic capsules per day, one probiotic capsule plus one placebo capsule per day, or two placebo capsules per day. Each probiotic capsule contained 50 billion CFU of a blend of probiotics (L acidophilus CL1285 and L casei LBC80R Bio-K+ CL1285). Results found a dose-response relationship of CDAD incidence, with 23.8% developing CDAD in the placebo group, 9.4% in the low-dose probiotic group, and 1.2% in the high-dose probiotic group. The authors concluded that a higher dose of a probiotic blend resulted in better clinical outcomes and fewer GI symptoms than did a lower dose.33
In a double-blind, placebo-controlled trial, 135 older hospitalized patients were randomized into one of two intervention groups during the course of antibiotic treatment and for one week after: one group consumed a 100 g (97 mL) probiotic yogurt drink twice per day (Actimel drink containing L casei, L bulgaricus, and S thermophilus); the other drank a placebo, sterile milkshake. In the probiotic group, zero patients tested positive for C diff, whereas nine patients in the control group developed C diff (P=0.001). The risk reduction for the occurrence of antibiotic-associated diarrhea was 22%, and the risk reduction for the occurrence of CDAD was 17%. Researchers estimated that the cost of the probiotic yogurt drinks were about $20 per patient. (Actimel costs about $0.60 per drink). The possible implications of this study are that a probiotic drink can be used routinely in older adults to reduce morbidity, mortality, and health care costs associated with C diff.34
In another study, subjects hospitalized with C diff were randomized to receive a probiotic supplement (2 X 10 billion CFU of L acidophilus and B bifidum) or a placebo capsule for 20 days while on antibiotics. Results showed that 46% of probiotic patients tested toxin-positive for C diff compared with 78% in the placebo group. Of those who tested positive for C diff and presented with diarrhea, 2.9% in the probiotic group developed CDAD compared with 7.25% in the placebo group.35
In a double-blind study, individuals with a history of C diff were assigned to a placebo group or a probiotic group that received 1 g/day of encapsulated S boulardii for 28 days. These individuals either were administered a course of high-dose vancomycin, low-dose vancomycin, or metronidazole antibiotics for 10 days. Results found that subjects in the high-dose vancomycin group had a significantly lower incidence of recurrent C diff (16.7%) when they consumed S boulardii compared with those who took a placebo (50%; P=0.05). However, no effects were found when probiotics were combined with low-dose vancomycin or metronidazole.36
In contrast, in a randomized, multicenter study, supplementation with probiotics (L acidophilus and two strains of Bifidobacteria) didn't affect incidence of CDAD compared with the placebo group.37 Some scientists believe that the results of well-conducted studies that didn't show positive effects of probiotics on antibiotic-associated diarrhea could be due to lack of probiotic activity, improper strain choice, or inadequate dosage.13
Few scientific studies have been conducted on the consumption of the fermented milk product kefir and its effect on C diff. However, one study found that individuals who experienced recurrent CDAD remained relapse-free after consuming 4 oz of kefir at every meal.38
Individuals receiving enteral feedings have been shown to have an increased risk of developing C diff. Possible reasons for this association is that tube-fed patients typically come in contact with health care workers at a greater frequency, are usually more acutely ill, are at higher risk of any type of complication, and are more often on antibiotics.39 Therefore, it's important to test for C diff in patients receiving enteral feedings who present with unexplained diarrhea. If the patient is positive for the toxin, it's typically recommended to continue the feeding as ordered unless clinical judgment indicates otherwise (for example, in cases of patients with abdominal distention, pain, inability to keep up with fluid losses, toxic megacolon, or colonic perforation). In fact, feeding the gut during periods of secretory diarrhea has been shown to improve enterocyte healing and enzyme activity maintenance. The addition of S boulardii to enteral formulas may be beneficial in the treatment of C diff.40 Some commercial enteral formulas already have a prebiotic fiber, known as NutraFlora, added. This prebiotic is fermented in the gut by the "good" bacteria (Bifidobacteria and Lactobacillistrains) while remaining unavailable to pathogenic bacteria.41
Dietitians' Role
There's evidence that the consumption of probiotics from both food and supplements can reduce the incidence and severity of antibiotic-associated diarrhea, C diff infections, and CDAD. Nutrition professionals can help guide at-risk individuals to choose appropriate probiotic-rich foods to incorporate into their diets. Dietitians also can help guide patients and other medical professionals in choosing a high-quality probiotic supplement. Future research in this area should focus on well-designed, double-blind, placebo-controlled studies with interventions using different probiotic food sources, such as kefir, on the risk of C diff and CDAD in the adult population.
— Mary Rodavich, MS, RD, LDN, is a dietitian and freelance writer based in Pittsburgh.
Learning Objectives
After completing this continuing education activity, nutrition professionals should be better be able to:
1. Counsel patients about the risk factors, symptoms, and treatment options for Clostridium difficile(C diff).
2. Assess the rationale for the use of probiotics in the prevention and treatment of C diff.
3. Recommend good food sources of probiotics.
CPE Monthly Examination
1. Clostridium difficile (C diff) accounts for what percentage of antibiotic-associated diarrhea?
a. 5% to 10%
b. 10% to 20%
c. 20% to 30%
d. 30% to 40%
2. Older adults are at greater risk of developing C diffdue to age-related effects on the defense system, the frequent use of antibiotics, and less frequent hospitalizations.
a. True
b. False
3. Probiotics can benefit the gut microbial environment by digesting food and competing for nutrients with pathogens.
a. True
b. False
4. Which of the following is not a dietary source of probiotics?
a. Kefir
b. Kimchi
c. Yogurt
d. Mushrooms
5. It's considered a better choice to consume probiotics in the form of which of the following?
a. Supplements
b. Food
c. Drugs
d. They're all equally beneficial
6. Greek yogurt is _____ in protein than regular yogurt and must contain at least ____ of protein (% m/m).
a. Lower, 2.7%
b. Lower, 5.6%
c. Higher, 2.7%
d. Higher, 5.6%
7. For adults receiving antibiotic treatment, current research indicates that probiotics can:
a. Increase the risk of developing a first episode of C diff-associated diarrhea
b. Increase the risk of developing a recurrent episode of C diff-associated diarrhea
c. Decrease the risk of developing both a first episode and recurrent episodes of C diffassociated-diarrhea
d. There is no association between probiotics and C diff
8. Common species and strains of probiotics used in commercial products include which of the following?
a. Bifidobacterium species, Streptococcus species, Saccharomyces boulardii
b. Bifidobacterium species, Streptococcus species, C diff
c. Bifidobacterium species, Streptococcus species, E coli
d. Bifidobacterium species, Streptococcus species, Salmonella
9. Which of the following is true regarding probiotics?
a. Probiotics are resistant to heat and acidity.
b. The shelf life of refrigerated probiotic products is about 12 months.
c. Probiotics can survive transit through the human gastrointestinal tract.
d. Probiotics produce more adverse side effects than prescription medications.
10. Nutrition professionals should encourage individuals when buying yogurt to choose those that have the Live & Active Cultures seal and contain less than ___ of fat and ____ of sugar per serving.
a. 1 g, 8 g
b. 2 g, 5 g
c. 3 g, 10 g
d. 4 g, 9 g
1. Making health care safer: stopping C. difficile infection. Centers for Disease Control and Prevention website. http://www.cdc.gov/vitalsigns/HAI/StoppingCdifficile/index.html. Updated March 6, 2012.
2. Cohen SH, Gerding DN, Johnson S, et al. Clinical practice guidelines for Clostridium difficile infection in adults: 2010 update by the Society for Healthcare Epidemiology of America (SHEA) and the Infectious Diseases Society of America (IDSA). Infect Control Hosp Epidemiol. 2010;31(5):431-455.
3. Buchner AM, Sonnenberg A. Medical diagnoses and procedures associated with Clostridium difficile colitis. Am J Gastroenterol. 2001;96(3):766-772.
4. McFarland LV. Epidemiology, risk factors and treatments for antibiotic-associated diarrhea. Dig Dis. 1998;16(5):292-307.
5. Mahan LK, Escott-Stump S. Krause's Food and Nutrition Therapy. 12th ed. St. Louis, MO: Elsevier Health Sciences; 2006.
6. Oldfield EC IV, Oldfield EC III, Johnson DA. Clinical update for the diagnosis and treatment of Clostridium difficile infection. World J Gastrointest Pharmacol Ther. 2014;5(1):1-26.
7. Simor AE. Diagnosis, management, and prevention of Clostridium difficile infection in long-term care facilities: a review. J Am Geriatr Soc. 2010;58(8):1556-1564.
8. Probiotic. Dictionary.com website. http://dictionary.reference.com/browse/probiotic?s=t. Accessed December 10, 2014.
9. Food and Agriculture Organization of the United Nations, World Health Organization Health and nutritional properties of probiotics in food including powder milk with live lactic acid bacteria. ftp://ftp.fao.org/docrep/fao/009/a0512e/a0512e00.pdf. Published October 2001. Accessed September 7, 2014.
10. Sanders ME, Lenoir-Wijnkoop I, Salminen S, et al. Probiotics and prebiotics: prospects for public health and nutritional recommendations. Ann N Y Acad Sci. 2014;1309:19-29.
11. Kopp-Hoolihan L. Prophylactic and therapeutic uses of probiotics: a review. J Am Diet Assoc. 2001;101(2):229-238.
12. Guarner F, Khan AG, Garisch J, et al. World Gastroenterology Organisation Global Guidelines: probiotics and prebiotics October 2011. J Clin Gastroenterol. 2012;46(6):468-481.
13. Douglas LC, Sanders ME. Probiotics and prebiotics in dietetics practice. J Am Diet Assoc. 2008;108(3):510-521.
14. Chandan RC, Kilara A. Manufacturing Yogurt and Fermented Milks. 2nd ed. Google eBook: John Wiley and Sons, Inc; 2013:443-448.
15. Bezkorovainy A. Probiotics: determinants of survival and growth in the gut. Am J Clin Nutr. 2001:73(2 Suppl):399S-405S.
16. Marcason W. Probiotics: where do we stand? J Acad Nutr Diet. 2013;113(10):1424.
17. Kapsak WR, Rehavi EB, Childs NM, White C. Functional foods: consumer attitudes, perceptions, and behaviors in a growing market. J Am Diet Assoc. 2011:111(6):804-810.
18. McDonald L. Eat your bacteria: understanding probiotics and live active cultures. Supermarket Savvy. https://nurturefoods.files.wordpress.com/2010/10/ssnlapr07.pdf. Accessed September 13, 2014.
19. Live and Active Culture Yogurt. National Yogurt Association website. http://aboutyogurt.com/live-culture. Accessed September 10, 2014.
20. El-Abbadi NH, Dao MC, Meydani SN. Yogurt: role in healthy and active aging. Am J Clin Nutr. 2014;99(5 suppl):1263S-1270S.
21. Yogurt, plain, low fat, 12 grams protein per 8 ounce. USDA National Nutrient Database for Standard Reference website. http://ndb.nal.usda.gov/ndb/foods/show/106?qlookup=Yogurt%2C+plain%2C+low+fat
%2C+12+grams+protein+per+8+ounce&fg=&format=&man=&lfacet=&max=25&new=1. Accessed November 13, 2014.
22. Martinez-Gonzalez MA, Sayon-Orea C, Ruiz-Canela M, de la Fuente C, Gea A, Bes-Rastrollo M. Yogurt consumption, weight change and risk of overweight/obesity: the SUN cohort study. Nutr Metab Cardiovasc Dis. 2014;24(11):1189-1196.
23. Wang H, Livingston KA, Fox CS, Meigs JB, Jacques PF. Yogurt consumption is associated with better diet quality and metabolic profile in American men and women. Nutr Res. 2013;33(1):18-26.
24. Lopez-Garcia E, Leon-Muñoz L, Guallar-Castillon P, Rodríguez-Artalejo F. Habitual yogurt consumption and health-related quality of life: a prospective cohort study. J Acad Nutr Diet. 2015;115(1):31-39.
25. Beniwal RS, Arena VC, Thomas L, et al. A randomized trial of yogurt for prevention of antibiotic-associated diarrhea. Dig Dis Sci. 2003;48(10):2077-2082.
26. de Vrese M, Kristen H, Rautenberg P, Laue C, Schrezenmeir J. Probiotic lactobacilli and bifidobacteria in a fermented milk product with added fruit preparation reduce antibiotic associated diarrhea and Helicobacter pylori activity. J Dairy Res. 2011;78(4):396-403.
27. Conway S, Hart A, Clark A, Harvey I. Does eating yogurt prevent antibiotic-associated diarrhoea? A placebo-controlled randomised controlled trial in general practice. Br J Gen Pract. 2007;57(545):953-959.
28. Williams MD, Ha CY, Ciorba MA. Probiotics as therapy in gastroenterology: a study of physician opinions and recommendations. J Clin Gastroenterol. 2010;44(9):631-636.
29. Boyanova L, Mitov I. Coadministration of probiotics with antibiotics: why, when and for how long? Expert Rev Anti Infect Ther. 2012;10(4):407-409.
30. Johnston BC, Ma SS, Goldenberg JZ, et al. Probiotics for the prevention of Clostridium difficile-associated diarrhea: a systematic review and meta-analysis. Ann Intern Med. 2012;157(12):878-888.
31. Pattani R, Palda VA, Hwang SW, Shah PS. Probiotics for the prevention of antibiotic-associated diarrhea and Clostridium difficile among hospitalized patients: systematic review and meta-analysis. Open Med. 2013;7(2):e56-e67.
32. Ouwehand AC, DongLian C, Weijian X, et al. Probiotics reduce symptoms of antibiotic use in a hospital setting: a randomized dose response study. Vaccine. 2014;32(4):458-463.
33. Gao XW, Mubasher M, Fang CY, Reifer C, Miller LE. Dose-response efficacy of a proprietary probiotic formula of Lactobacillus acidophilus CL1285 and Lactobacillus casei LBC80R for antibiotic-associated diarrhea and Clostridium difficile-associated diarrhea prophylaxis in adult patients. Am J Gastroenterol. 2010;105(7):1636-1641.
34. Hickson M, D'Souza AL, Muthu N, et al. Use of probiotic Lactobacillus preparation to prevent diarrhoea associated with antibiotics: randomised double blind placebo controlled trial. BMJ. 2007;335(7610):80.
35. Plummer S, Weaver MA, Harris JC, Dee P, Hunter J. Clostridium difficile pilot study: effects of probiotic supplementation on the incidence of C. difficile diarrhoea. Int Microbiol. 2004;7(1):59-62.
36. Surawicz CM, McFarland LV, Greenberg RN, et al. The search for a better treatment for recurrent Clostridium difficile disease: use of high-dose vancomycin combined with Saccharomyces boulardii. Clin Infect Dis. 2000;31(4):1012-1017.
37. Allen SJ, Wareham K, Wang D, et al. A high-dose preparation of lactobacilli and bifidobacteria in the prevention of antibiotic-associated and Clostridium difficile diarrhoea in older people admitted to hospital: a multicentre, randomised, double-blind, placebo-controlled, parallel arm trial (PLACIDE). Health Technol Assess. 2013;17(57):1-140.
38. Bakken JS. Resolution of recurrent Clostridium difficile-associated diarrhea using staggered antibiotic withdrawal and kefir. Minn Med. 2009;92(7):38-40.
39. O'Keefe SJ. Tube feeding, the microbiota, and Clostridium difficile infection. World J Gastroenterol. 2010;16(2):139-142.
40. DeLegge MH, Berry A. Enteral Feeding: Should it be continued in the patient with Clostridium difficile Enterocolitis? Pract Gastroenterol. 2009;33(3):40-49.
41. NutraFlora — delivers the most effective, pure prebiotic fiber benefits. Ingredion website. http://www.ingredion.us/YogurtCapabilities/Documents/NUTRAFLORA_Ingredient_Brochure-R10-lowres.pdf
Handout
Tips for Incorporating Probiotics Into the Diet
- Dietary sources of probiotics include fermented milk products (such as yogurt, kefir, and buttermilk), fermented vegetables (such as kimchi and sauerkraut), and fermented soy products (such as miso and tempeh).
- Look for food sources with the Live & Active Cultures seal established by the National Yogurt Association.
- To ensure the highest levels of probiotics, consume food products as close to the manufacturing date as possible.
- Consuming food sources of probiotics rather than supplements is recognized as a better choice due to the synergistic effect between probiotics and other nutrients found in food.
- If probiotic products and supplements are chosen, take capsules in combination with food. This decreases the acidity of the stomach, which is a more favorable environment for probiotic survival.
- Consume food sources of probiotics on a daily basis to maintain their health benefits.
- Choose probiotic products that are lower in fat (≤3 g fat/serving) and contain little added sugar (≤10 g sugar/serving).
- Yogurt can serve as a medium for mixing in other healthful foods, such as granola, nuts, seeds, fruits, cold cereals, graham crackers, honey, cinnamon, jams, and peanut butter.
- Recommending Greek yogurt may be beneficial for individuals looking for a yogurt that's higher in protein and lower in fat.
- Individuals who are immunocompromised, recovering from surgery, or have compromised gut integrity are at greater risk of infection and should take probiotics under medical supervision.
- Those receiving tube feedings should look for enteral formulas with probiotics, prebiotics, or NutraFlora already added.