Today’s Dietitian
Vol. 18, No. 11, P. 18
Many patients take a holistic approach to help maintain sight long term.
Glaucoma is an inadequately understood and insidious disease. In the most common form, primary open-angle glaucoma, vision is eroded slowly and without pain, starting first with side vision and then central vision—potentially resulting in blindness. For this reason, it’s often called “the sneak thief of sight.” Although it’s more common in older people, it can start at any age.
Glaucoma generally isn’t curable, but medications and surgery can help slow disease progression. A healthful lifestyle, including good nutrition, regular exercise, stress management, and avoiding smoking also may be protective. Growing evidence suggests certain complementary and alternative medicine (CAM) therapies may be good adjuncts to conventional care.
Approximately one in nine glaucoma patients uses CAM therapies; herbal remedies and nutritional supplements are most common.1 A small percentage of glaucoma patients report trying acupuncture, and some wonder whether medical marijuana would help.2 Dietitians and eye health professionals must keep abreast of such therapies to ensure a collaborative partnership in which patients feel comfortable discussing such options.
Glaucoma Basics
Although the precise cause of glaucoma is poorly understood, a major risk factor for glaucoma is high eye pressure or intraocular pressure (IOP), which is the main target of treatment in open-angle glaucoma.3 Other risk factors for glaucoma include oxidative damage and poor blood flow to the optic nerve, which transmits visual information from the eye to the brain.
Just as car tires need the right amount of pressure to run well, so do the eyes. If the pressure in the eyes is too high (due to an imbalance between aqueous humor formation and its drainage from the eye), it can push against the optic nerve, slowly wearing away the nerve cells required for vision. However, a person with high eye pressure won’t necessarily develop glaucoma. And a person with normal eye pressure—generally defined as 12 to 21 mm Hg—still can develop glaucoma.4
Prescription eye drops, laser therapies, and surgical procedures are the typical ways to lower eye pressure and improve fluid drainage in glaucoma. However, for some people these therapies aren’t enough, and a small number of patients may refuse conventional treatment. About 10% of people with glaucoma who receive proper treatment still experience vision loss.5 In addition, some people don’t tolerate glaucoma eye drops well.6
Dietary Supplements
Nutritional supplements for eye health are one type of complementary treatment glaucoma patients can consider. “There are a number of supplements that appear to provide benefits, both in terms of optic nerve protection and pressure lowering, plus they have a relatively good side effect profile,” says David Richardson, MD, an ophthalmologist specializing in the treatment of cataracts and glaucoma in San Marino, California.
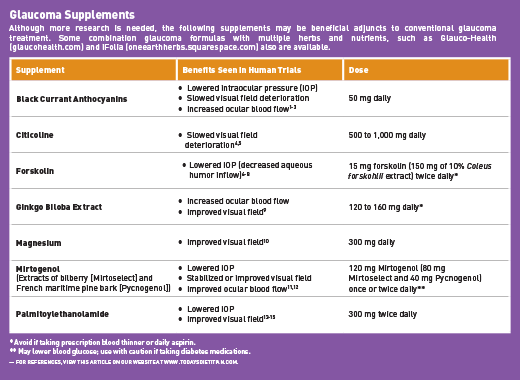
“In general, I try to tailor the supplement to the individual patient because there’s evidence supporting well over a dozen different supplements in the treatment of glaucoma,” Richardson says. For example, if a patient has chronic pain, a palmitoylethanolamide (PEA) supplement could help with that as well as the eyes.7 Additional supplements he recommends based on glaucoma research include Mirtogenol, Ginkgo biloba extract, and citicoline, among others. Some of the more promising supplements for glaucoma are summarized in the table below.
“My preference is to start supplements when I’m concerned about early glaucoma but there’s not yet vision loss,” Richardson says. “Once there’s been a significant amount of damage to the optic nerve, then supplements truly become a supplement to more traditional glaucoma therapies. Supplements also may complement treatment postsurgery, in some cases enabling patients to avoid going back on eye drops.”
On their own, supplements such as PEA and Mirtogenol typically don’t lower IOP to the same extent as medications, laser treatment, or surgery, and it may take a few months or longer to really see a benefit, Richardson says. Studies suggest many eye health supplements, such as Ginkgo biloba extract and citicoline, generally are of greater help in protecting the optic nerve.8,9 Unfortunately, because of the slow, progressive nature of glaucoma, protective effects of supplements on the optic nerve can be challenging to measure.
If you introduce more than one supplement at a time, it will be difficult to know which, if any, is helping. If a patient desires an aggressive supplement strategy, Richardson suggests introducing no more than one new supplement per week to at least ensure there aren’t any side effects.
Medical Marijuana
Since several states have legalized medical marijuana (cannabis), including for glaucoma use, it has received increasing interest from glaucoma patients.10 “Marijuana lowers eye pressure, but it’s only effective for about four hours,” says Jeff Anshel, OD, founder and past president of the Ocular Nutrition Society and author of What You Must Know About Food and Supplements for Optimal Vision Care: Ocular Nutrition Handbook. So, a person would need to smoke a marijuana cigarette as many as eight to 10 times a day in order to control IOP over 24 hours.11 “Given marijuana’s euphoric side effect, that would make it very difficult to be functional during the day,” Anshel says.
Moreover, it’s not just the average IOP that must be considered but also how much eye pressure fluctuates. “Too much fluctuation in IOP can cause damage,” Richardson says. “If you’re taking something that lowers the pressure for only a few hours, you’re going to increase the amount of fluctuation that occurs. So, you’ll have highs and lows, and that can be more damaging to the optic nerve.”
Using medical marijuana also can increase heart rate and lower blood pressure; if blood pressure is too low, there’s less blood flow to the optic nerve, which could deprive it of oxygen and nutrients.11 For these reasons, its use generally isn’t recommended for glaucoma.
Marijuana Alternatives
Preliminary animal research suggests a nonpsychoactive part of cannabis, cannabidiol (CBD), may help in glaucoma, but human clinical trials are needed.12-14 “CBD is a neuroprotectant and improves blood flow to the optic nerve,” says Anshel, who consults for CV Sciences, a CBD supplement manufacturer. Because CBD doesn’t have a euphoric side effect, it’s legal to use CBD supplements regardless of where a person lives.
Another alternative to marijuana is PEA, which is sold as the supplement PeaPure (available at rs4supplements.com/en). “It’s a natural chemical that occurs in our brains and works via a similar pathway as marijuana,” Richardson says. “So, you get the eye pressure-lowering and pain-reducing benefits without the high.” Some foods, such as peanuts, egg yolks, and soybeans also contain PEA.15
PEA is naturally present in the part of the eye that produces aqueous fluid, and it has both anti-inflammatory and neuroprotective actions.16 Interestingly, people with glaucoma have less PEA in their eyes. This suggests that either less is produced and/or more is used up.
“PEA supplements are good for almost anyone with glaucoma,” Richardson says. Placebo-controlled human trials suggest PEA supplements (300 mg twice daily) may lower IOP in both normal and high-pressure glaucoma and may help improve visual field.7,15-17
Acupuncture
Acupuncture is an ancient Chinese medicine technique for balancing the flow of energy in the body and involves inserting extremely thin needles through the skin at specific points. Of the limited number of studies on acupuncture for glaucoma, some, but not all, report beneficial effects in reducing IOP, improving visual acuity, and opening the visual field.18,19 Drawing conclusions from these studies is challenging because of differing methodologies and the variability in specific acupuncture points used.
Furthermore, an evaluation of acupuncture treatment published in the American Journal of Ophthalmology in 2015 reported that acupuncture temporarily might increase IOP slightly, immediately after a treatment session.20 This is because acupuncture typically is administered while the patient is lying down; this, by itself, often can elevate IOP slightly (usually no more than 2 to 3 mm Hg), says Andy Rosenfarb, ND, LAc, founder and clinical director of Acupuncture Health Associates in Westfield, New Jersey, and author of Healing Your Eyes With Chinese Medicine: Acupuncture, Acupressure, & Chinese Herbs. Someone unfamiliar with acupuncture could misinterpret this as counterproductive to glaucoma management.
Over the past few decades, Rosenfarb has honed his skills and knowledge in using acupuncture for glaucoma treatment by collaborating with integrative neurologists, eye doctors, and glaucoma specialists around the world. In the process, he has determined which acupuncture systems are most effective for eye health and glaucoma. Rosenfarb believes that the methods he has developed can help improve blood flow to the optic nerve and help preserve its health and function, which can help protect vision in those with glaucoma.
“I typically see measurable results in 10 acupuncture treatments,” he says. He assesses this through conventional methods, including testing visual fields and measuring eye pressure, among other standard tests. However, he says not everyone with glaucoma responds to acupuncture treatment, and it should be viewed as an integrative strategy for long-term vision preservation rather than a cure for glaucoma. Glaucoma patients who are considering trying acupuncture should ask practitioners about their level of experience in treating glaucoma and how they monitor progress.
Support a Collaborative Approach
Patients need to feel comfortable disclosing their use of CAM therapies so they can have a nonjudgmental, open conversation with providers. One survey found that 62% of glaucoma patients using CAM therapies didn’t disclose this to their doctor; this suggests there’s apprehension in sharing this information with conventional practitioners. Fortunately, most patients who use complementary therapies tend to do so in conjunction with traditional therapies, an important consideration in protecting vision.1
“Since patients can’t tell on their own whether glaucoma is getting better or worse, they need glaucoma testing on a regular basis, which may vary from every three months to annually, depending on the stage and level of control of their glaucoma,” Richardson says. That requires a true partnership. Being open-minded and knowledgeable about CAM therapies in glaucoma will facilitate that, and dietitians can help guide exploration of dietary supplement strategies.
— Marsha McCulloch, MS, RD, LD, LN, is a nutrition writer and consultant in South Dakota.
References
1. Wan MJ, Daniel S, Kassam F, et al. Survey of complementary and alternative medicine use in glaucoma patients. J Glaucoma. 2012;21(2):79-82.
2. Rhee DJ, Spaeth GL, Myers JS, et al. Prevalence of the use of complementary and alternative medicine for glaucoma. Ophthalmology. 2002;109(3):438-443.
3. Primary open-angle glaucoma (POAG). The Glaucoma Foundation website. https://www.glaucomafoundation.org/Primary_Open-Angle_Glaucoma.htm. Accessed September 7, 2016.
4. Tsai JC. High eye pressure and glaucoma. Glaucoma Research Foundation website. http://www.glaucoma.org/gleams/high-eye-pressure-and-glaucoma.php. Updated May 3, 2016. Accessed September 6, 2016.
5. Glaucoma facts and stats. Glaucoma Research Foundation website. http://www.glaucoma.org/glaucoma/glaucoma-facts-and-stats.php. Updated September 7, 2016. Accessed September 7, 2016.
6. Inoue K. Managing adverse effects of glaucoma medications. Clin Ophthalmol. 2014;8:903-913.
7. Keppel-Hesselink JM, Costagliola C, Fakhry J, Kopsky DJ. Palmitoylethanolamide, a natural retinoprotectant: its putative relevance for the treatment of glaucoma and diabetic retinopathy. J Ophthalmol. 2015;2015:430596.
8. Doozandeh A, Yazdani S. Neuroprotection in glaucoma. J Ophthalmic Vis Res. 2016;11(2):209-220.
9. Roberti G, Tanga L, Michelessi M, et al. Cytidine 5′-diphosphocholine (citicoline) in glaucoma: rationale of its use, current evidence and future perspectives. Int J Mol Sci. 2015;16(12):28401-28417.
10. Wilkinson ST, Yarnell S, Radhakrishnan R, Ball SA, D’Souza DC. Marijuana legalization: impact on physicians and public health. Annu Rev Med. 2016;67:453-466.
11. American Academy of Ophthalmology Complementary Therapy Task Force, Hoskins Center for Quality Eye Care. Marijuana in the treatment of glaucoma CTA — 2014. American Academy of Ophthalmology website. http://www.aao.org/complimentary-therapy-assessment/marijuana-in-treatment-of-glaucoma-cta–may-2003. Updated June 2014.
12. El-Remessy AB, Khalil IE, Matragoon S, et al. Neuroprotective effect of Delta 9-tetrahydrocannabinol and cannabidiol in N-methyl-D-aspartate-induced retinal neurotoxicity. Am J Pathol. 2003;163(5):1997-2008.
13. Tomida I, Pertwee RG, Azuara-Blanco A. Cannabinoids and glaucoma. Br J Ophthalmol. 2004;88(5):708-713.
14. Yazulla S. Endocannabinoids in the retina: from marijuana to neuroprotection. Prog Retin Eye Res. 2008;27(5):501-526.
15. Hesselink JM. Evolution in pharmacologic thinking around the natural analgesic palmitoylethanolamide: from nonspecific resistance to PPAR-alpha agonist and effective nutraceutical. J Pain Res. 2013;6:625-634.
16. Costagliola C, Romano MR, dell’Omo R, Russo A, Mastropasqud R, Semero F. Effect of palmitoylethanolamide on visual field damage progression in normal tension glaucoma patients: results of an open-label six-month follow-up. J Med Food. 2014;17(9):949-954.
17. Gagliano C, Ortisi E, Pulvirenti L, et al. Ocular hypotensive effect of oral palmitoyl-ethanolamide: a clinical trial. Invest Ophthalmol Vis Sci. 2011;52(9):6096-6100.
18. Rom E. Sensory stimulation for lowering intraocular pressure, improving blood flow to the optic nerve and neuroprotection in primary open-angle glaucoma. Acupunct Med. 2013;31(4):416-421.
19. Yeh TY,Lin JC, Liu CF. Effect of transcutaneous nerve stimulation through acupoints of Pucan (BL 61) and Shenmai (BL 62) on intraocular pressure in patients with glaucoma: a randomized controlled trial. J Tradit Chin Med. 2016;36(1):51-56.
20. Law SK, Lowe S, Law SM, Giaconi JA, Coleman AL, Caprioli J. Prospective evaluation of acupuncture as treatment of glaucoma. Am J Ophthalmol. 2015;160(2):256-265.


